AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.
Question 1
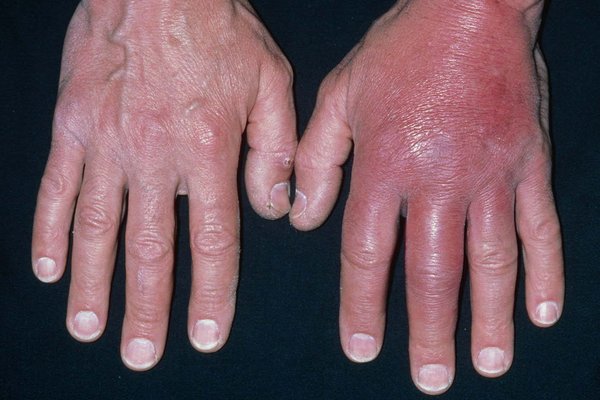
A 51-year-old man presents to the hospital with a swollen hand shown in the following photograph. He was doing some gardening at his courtyard yesterday when he had his left index finger injured. This morning, he noticed that his left hand is tender, swollen, and red. On examination, he has a blood pressure of 134/78 mmHg, pulse of 88, respiratory rate of 16 breaths/min and temperature of 38.1°C. Which one of the following is the most appropriate next step in management?
A) Ultrasound of the hand
B) MRI of the hand
C) Admission to the hospital and commencement of intravenous antibiotics
D) CT scan of the hand
E) Discharge him home on oral antibiotics and review in 24-48 hours
Question 2
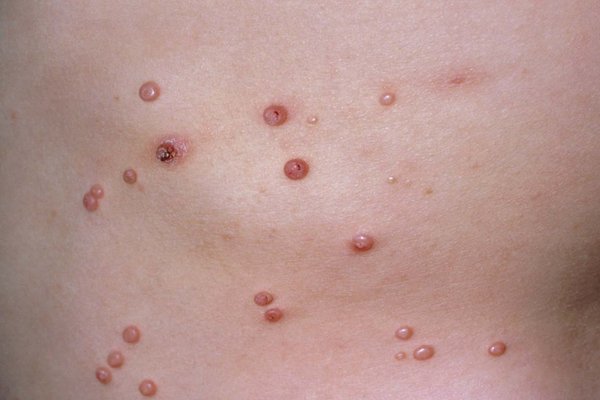
A 7-year-old girl, Evie, is brought to your general practice by her mother who is concerned about a rash she has developed, as shown in the following photograph. The rash appeared almost two months ago on her abdomen and has spread to the extent evident in the photo. There is no complaint of pain or itching, but a few lesions have ulcerated (one shown in the photograph). Evie is otherwise healthy and has not had any serious illnesses so far. Her growth charts are all normal. Physical examination is otherwise normal. She goes to school and has two younger brothers and sisters at home. Which one of the following is a correct advice to give?
A) She should be excluded from school until the resolution of the rash
B) She can go to school but should use separated towel and other personal items
C) She should be given oral acyclovir
D) Cryotherapy with liquid nitrogen is the treatment of choice for the rash
E) She should use topical steroids
Question 3
A 60-year-old man presents to your clinic with complaints of fever and a painful swollen right thigh. He has diabetes well controlled on metformin 500 mg 8-hourly and hypertension for which he is taking valsartan 80 mg daily. He is on atorvastatin 20 mg daily for hypercholesterolemia as well. His recent medical history is remarkable for deep vein thrombosis (DVT) of his right leg, for which he is currently on warfarin. One week ago, he was admitted to the hospital after one episode of syncope and started on amiodarone after he was diagnosed with ventricular tachycardia (VT). Physical examination is remarkable for a temperature of 38.3°C and a warm swollen tender right thigh that is erythematous. Right thigh circumference is 3 cm greater than that of the left thigh. Which one of the following could be the most likely cause of this presentation?
A) Deep vein thrombosis (DVT)
B) Cellulitis
C) Drug interaction
D) Hematoma
E) Rhabdomyolysis


Author – Dr. James Whitfield (MBBS, FRACGP)
With over 30 years in primary care, Dr. James Whitfield is a highly experienced GP providing comprehensive medical services for individuals and families. He has a strong background in chronic disease management, preventive health, and minor surgical procedures.