AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.
Question 1
A 27-year-old man presents with extremely itchy rash on his buttocks and elbows as shown in the following photograph. He has long-standing history of celiac disease. He was also diagnosed with major depression seven months ago for which he is under treatment with Zoloft. Which one of the following could be the most likely diagnosis?
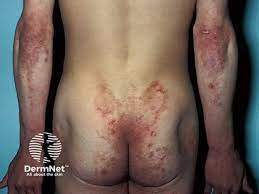
A) Linear IgA dermatosis
B) Neurotic excoriation
C) SSRI-induced dermatitis
D) Scabies
E) Dermatitis herpetiform
Question 2
A 2-year-old boy is brought to the emergency department, by his mother, after he developed a rash following a bee sting 20 minutes ago. The appearance of the rash is shown in the following photograph. On examination, there is no breathlessness, wheezing, abdominal pain, or hemodynamic instability. Which one of the following is the most appropriate management?
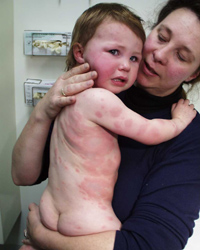
A) Intravenous epinephrine
B) Intravenous diphenhydramine
C) Intramuscular epinephrine
D) Oral promethazine
E) Oral corticosteroids
Question 3
A 17-year-old girl presents to your GP practice with redness and swelling of the sun-exposed areas of her face after she spent 60 minutes in the sun. She is on treatment for acne. On examination, erythema and edema of the sun-exposed areas of her face, neck and upper chest are noted. There are bullae all over the area. Which one of the following is the most likely diagnosis?
A) Doxycycline phototoxicity
B) Allergic contact dermatitis
C) Erythromycin phototoxicity
D) Stevens – Johnson syndrome
E) Benzoyl peroxide phototoxicity


Author – Dr. James Whitfield (MBBS, FRACGP)
With over 30 years in primary care, Dr. James Whitfield is a highly experienced GP providing comprehensive medical services for individuals and families. He has a strong background in chronic disease management, preventive health, and minor surgical procedures.