AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.
Question 1
A 15-year-old boy is brought by his parents because of a painless swelling just above his left knee. The swelling has been present for over a year and has slowly increased in size. There is no history of trauma, fever, or weight loss. On examination, there is a hard, immobile, non-tender mass arising from the medial aspect of the distal femur. The overlying skin is normal. X-ray of the knee is shown below.
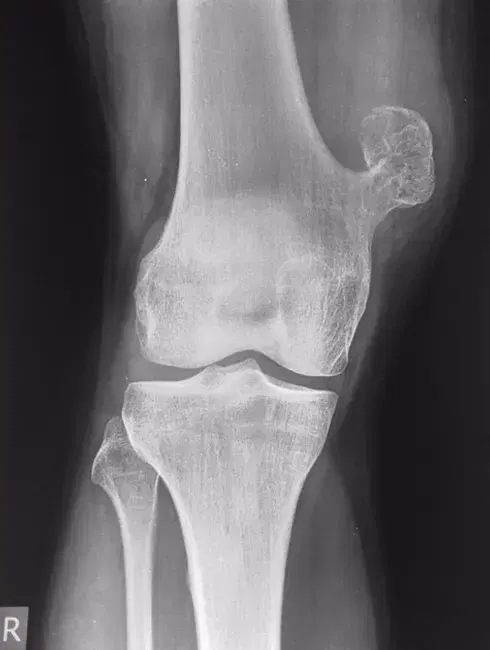
Which of the following is the most likely diagnosis?
A) Osteosarcoma
B) Osteochondroma
C) Osteoid osteoma
D) Fibrous dysplasia
E) Chondrosarcoma
Question 2
A 38-year-old woman presents with mild swelling and occasional discomfort in her left index finger for the past 6 months. She denies any trauma, fever, or constitutional symptoms. On examination, there is a firm, non-tender swelling over the distal phalanx. There is no redness or warmth. X-ray of the hand is shown below.
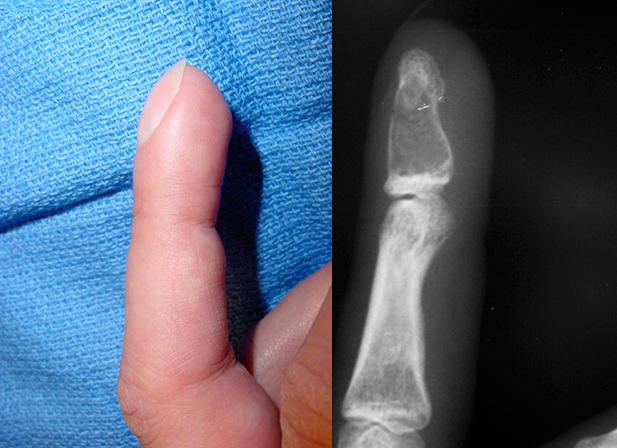
Which of the following is the most likely diagnosis?
A) Chondrosarcoma
B) Osteoid osteoma
C) Enchondroma
D) Giant cell tumor
E) Fibrous dysplasia
Question 3
A 17-year-old girl presents with intermittent dull pain in her right thigh for the past 8 months. She reports occasional limping but denies trauma, fever, or weight loss. On examination, there is mild tenderness over the proximal femur but no swelling or redness. X-ray of the femur is given below.
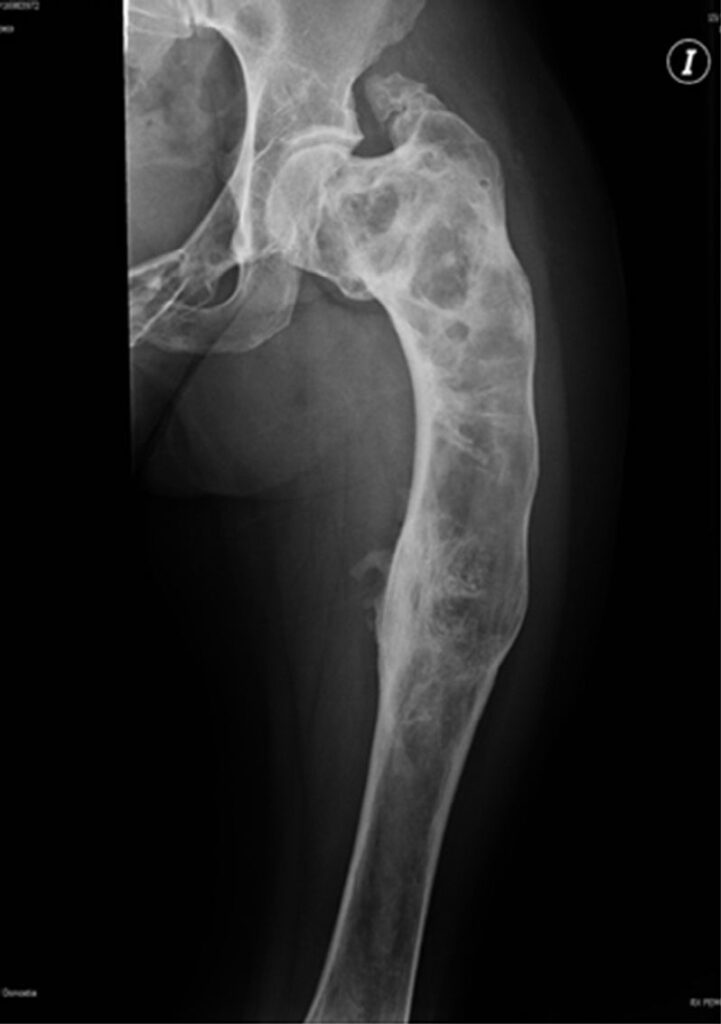
Which of the following is the most likely diagnosis?
A) Fibrous dysplasia
B) Osteosarcoma
C) Non-ossifying fibroma
D) Aneurysmal bone cyst
E) Ewing sarcoma