AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.

Written by Dr. Andrew McAllister
(MBBS, FRACS) – Surgeon
Question 1
In which one of the following conditions of the colon, occurrence of malignant changes is most likely?
A) Adenomatous polyp
B) Melanosis coli
C) Diverticulitis
D) Ulcerative colitis
E) Familial polyposis coli
Question 2
A 32-year-old woman, who has just recently migrated from Somalia to Australia, presents to your practice with complaint of severe anal pain, particularly on defecation, for the past 3 months. She mentions that at times she notices blood streaking her stool or dripping in the toilet bowl after a painful bowel movement. Examination, along with the history, confirms the diagnosis of anal fissure.
Which one of the following options is the most expected predisposing factor for this presentation in this patient?
A) Rectal cancer
B) Hemorrhoids
C) Perianal abscess
D) Rectal schistosomiasis
E) High-fiber diet
Question 3
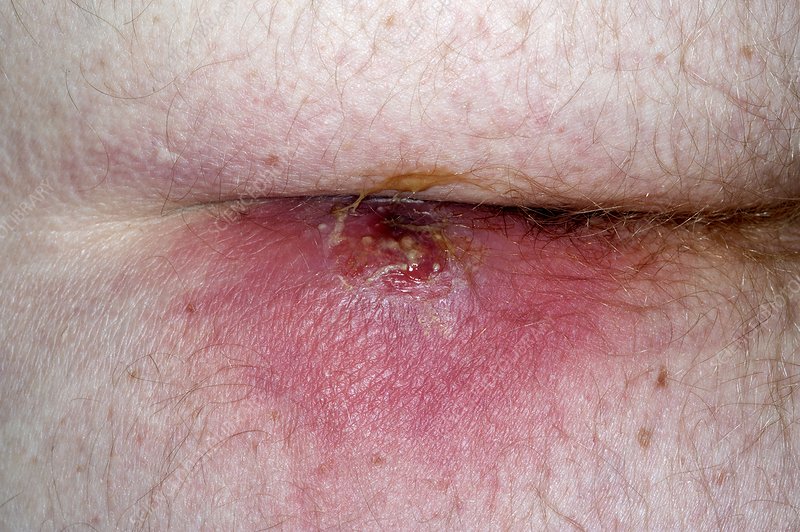
A 27-year-old woman presents to the Emergency Department with severe perianal pain started 10 hours ago that has increased progressively since then. The pain is exquisite and the patient is unable to sit. The anal region is shown in the following photograph.
Which one of the following would be the most important part of management for this patient?
A) Incision under local anesthesia
B) Hemorrhoidectomy under general anesthesia
C) Topical antihemorrhoid agents
D) Antibiotics
E) Hemorrhoidectomy under topical anesthesia


