AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.

Written by Dr. James Whitfield (MBBS, FRACGP) – General Practitioner
Question 1
A 48-year-old woman presents to the emergency department with a sudden, severe headache that she describes as “the worst headache of my life.” The pain began abruptly while she was exercising at the gym. She vomited shortly after the onset and has been increasingly photophobic. On examination, she is alert but distressed. Neck flexion is painful, and her blood pressure is 162/98 mmHg. A non-contrast CT brain is performed and shown below.
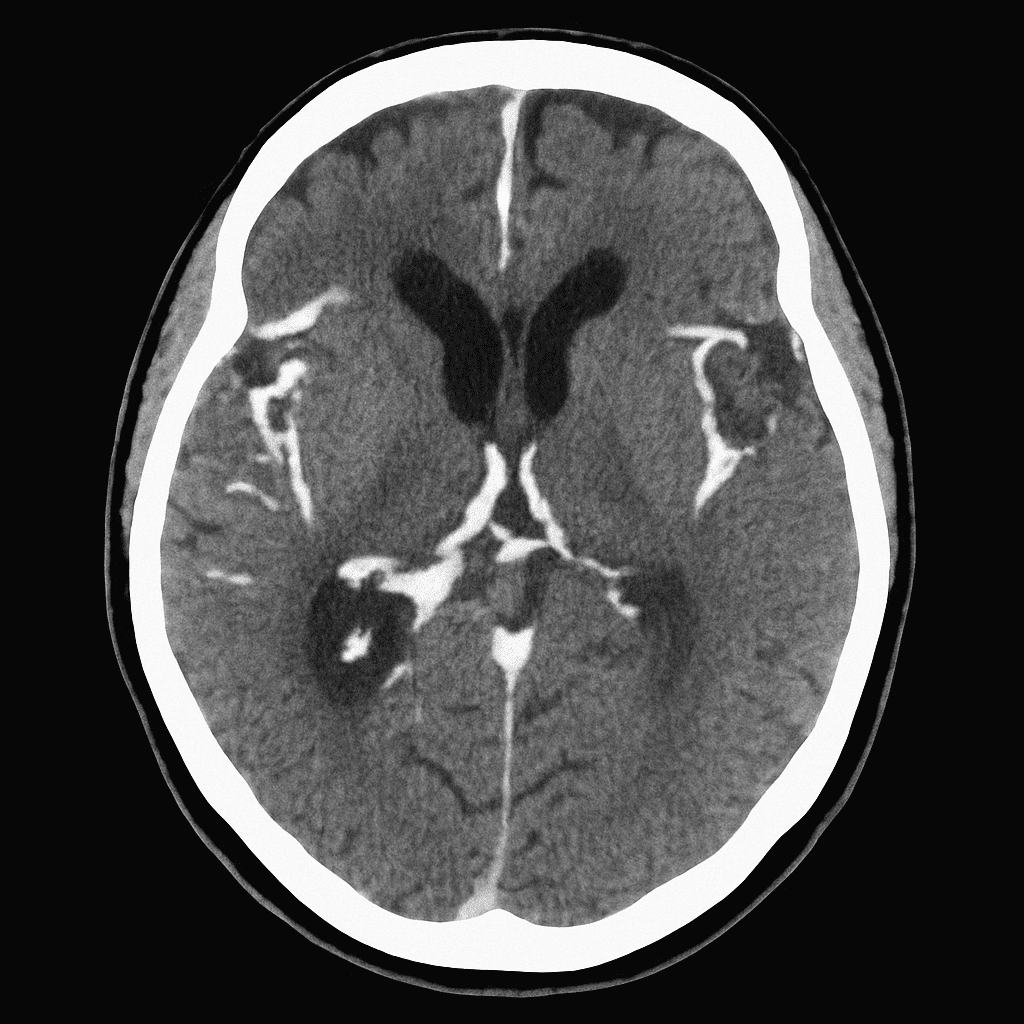
Which of the following is the most likely diagnosis?
A) Acute migraine
B) Subarachnoid haemorrhage
C) Intracerebral haemorrhage
D) Viral meningitis
E) Acute ischaemic stroke
Question 2
A 76-year-old man is brought to the emergency department after being found confused at home. He lives alone and his neighbour reports that he had a minor fall about two weeks ago but did not seek medical attention. On examination, he is slow to respond and has a mild right-sided weakness. His vital signs are stable. A non-contrast CT brain is performed and shown below.
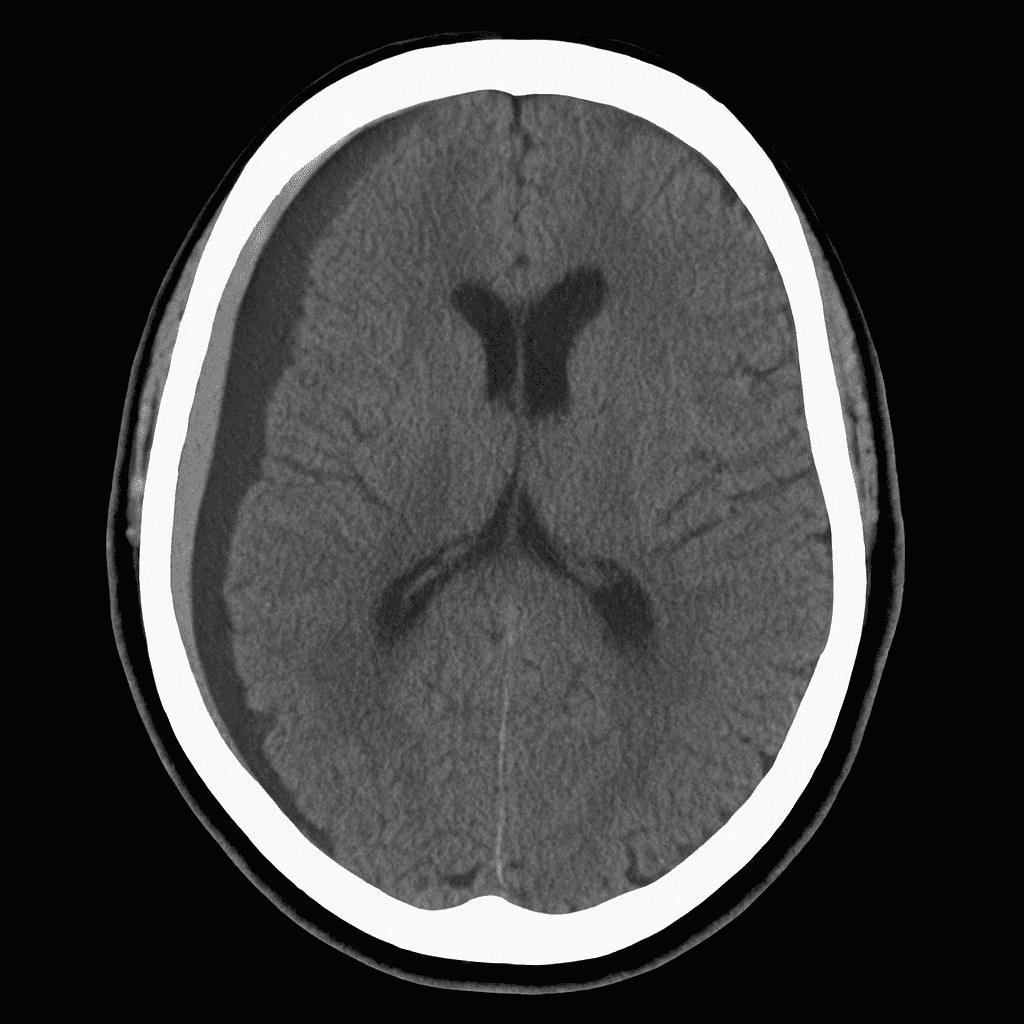
Which of the following is the most likely diagnosis?
A) Acute intracerebral haemorrhage
B) Chronic subdural haematoma
C) Extradural haematoma
D) Acute ischaemic stroke
E) Brain abscess
Question 3
A 24-year-old man is brought to the emergency department after being struck on the side of the head during a motorbike accident. He was initially unconscious for a few minutes but became fully alert on arrival to the scene. Over the next hour, he develops worsening headache, repeated vomiting, and increasing drowsiness. On examination, his GCS has dropped from 15 to 11. A non-contrast CT brain is performed and shown below.
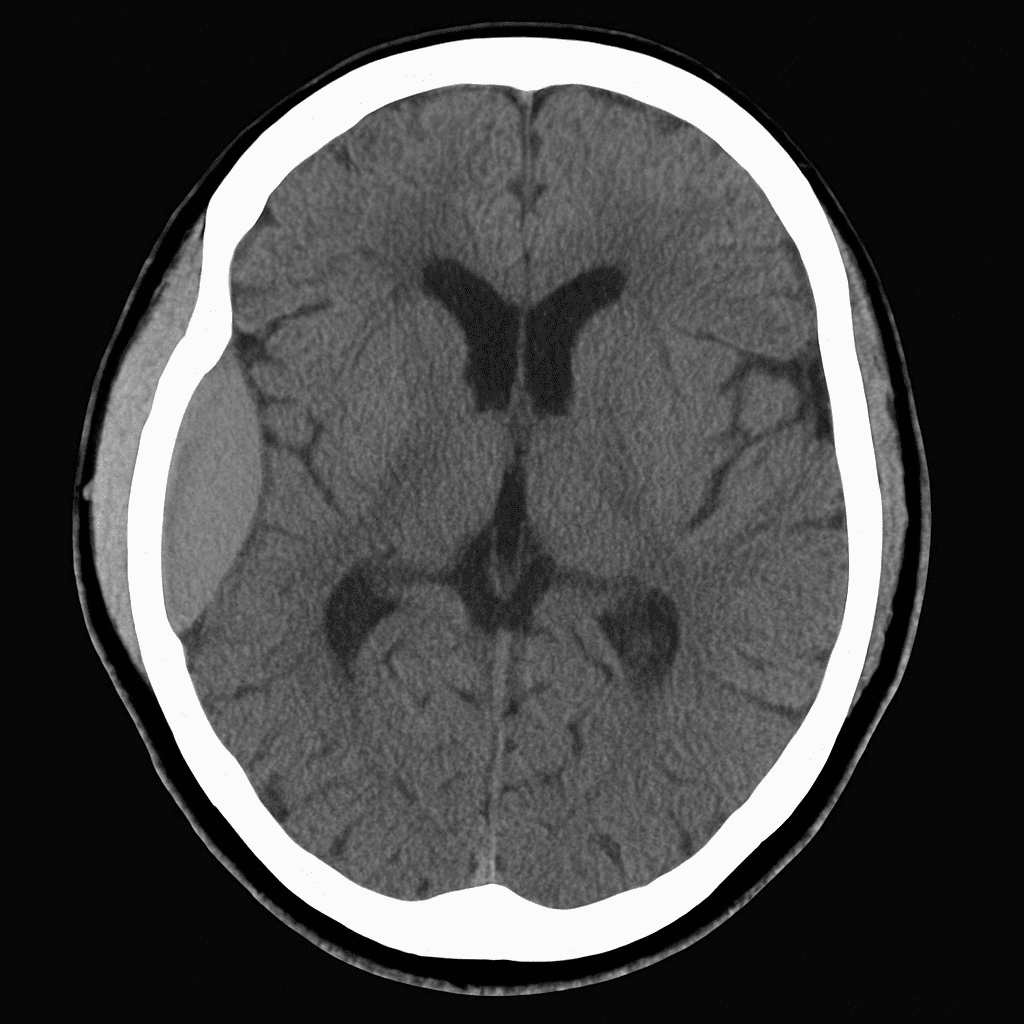
Which of the following is the most likely diagnosis?
A) Acute subdural haematoma
B) Extradural haematoma
C) Acute intracerebral haemorrhage
D) Traumatic subarachnoid haemorrhage
E) Cerebral contusion


