AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.
Question 1
An 80-year-old woman presents to your GP clinic with ‘funny spots’ affecting her right vision. Over the past week, she has noticed a number of flashes and floaters in the visual field of the right eye. On physical examination, visual acuity and fields are normal. Which one of the following could be the most likely diagnosis?
A) Vitreous hemorrhage
B) Retinal detachment
C) Depression
D) Optic neuritis
E) Posterior vitreous detachment
Question 2
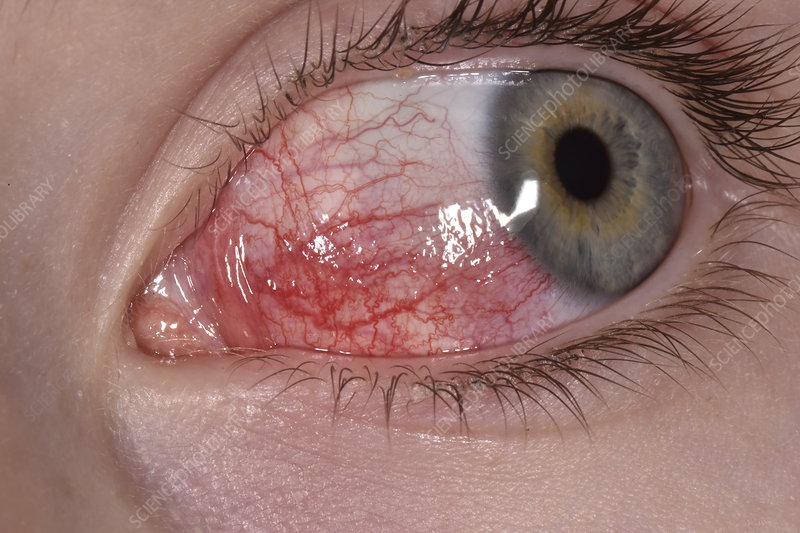
A 26-year-old woman presents with red right eye since this morning. For the past few hours she also has had mild discomfort and irritation of the eye. She denies any discharge or itchiness. On examination, eye movements, orbital pressure and visual acuity are normal. Cornea shows no abnormality and has preserved light and red reflexes. A funduscopic exam reveals no retinal abnormality either. She has unaffected visual acuity. There is a patchy redness of the sclera as shown in the following photograph. Which one of the following would be the most appropriate eye drop to consider for her?
A) Ketotifen
B) Hypomellose
C) Sodium cromoglycate
D) Prednisolone
E) Chloramphenicol
Question 3
A 48-year-old woman presents to your practice with complaints of a painful red eye and decreased vision that has started and progressed since 3 days ago. On examination, the left eye is red, but the cornea is normal in appearance with preserved light and red reflexes. Vision is 4/12 on the left and 10/12 on the right side. The orbit movement are preserved and painless. Which one of the following could be the most likely diagnosis?
A) Glaucoma
B) Conjunctivitis
C) Blepharitis
D) Uveitis
E) Keratitis

