AMC Wise will be offline from 12.00am, 7/2/2026 to 8.00am 9/2/2026 for a scheduled maintenance.
Question 1
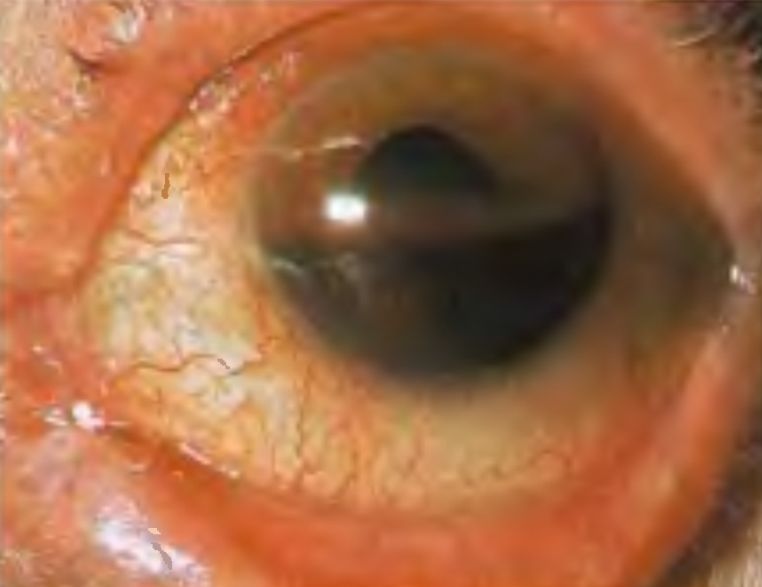
A 38-year-old woman presents to the emergency department after getting hit in her right eye with a squash ball in a match. On examination, the visual acuity of the affected eye is decreased. The eye is shown in the accompanying photograph. Which one of the following is the most appropriate next step in management?
A) Application of an eye patch.
B) Topical antibiotics.
C) Urgent referral to an ophthalmologist.
D) Evacuation of the blood under local anesthesia.
E) Reassurance as it resolves within 5 to 7 days.
Question 2
A 42-year-old machinist engineer comes to the emergency department with foreign body in his left eye. On examination, a metal speck is found stuck in the cornea. Which one of the following is the most appropriate management?
A) Remove the foreign body under local anesthesia.
B) Obtain an orbital X-ray.
C) Refer the patient to an ophthalmologist.
D) Cover the eye with a pad.
E) Remove the foreign body under general anesthesia.
Question 3
A 21-year-old woman presents to your office with itchy and watery eyes. Her symptoms started 2 days ago with redness of both eyes, lacrimation and itching. She wears contact lenses. On examination, her upper and lower lids are erythematous bilaterally. Which one of the following, if in history, is most consistent with the diagnosis?
A) Mucopurulent discharge.
B) A lump in the upper eyelid.
C) Reduced visual acuity.
D) Using a new preserving solution for her contact lenses.
E) Bacterial conjunctivitis 3 months ago.

